Patient Perspective: LillyAnn’s Heart
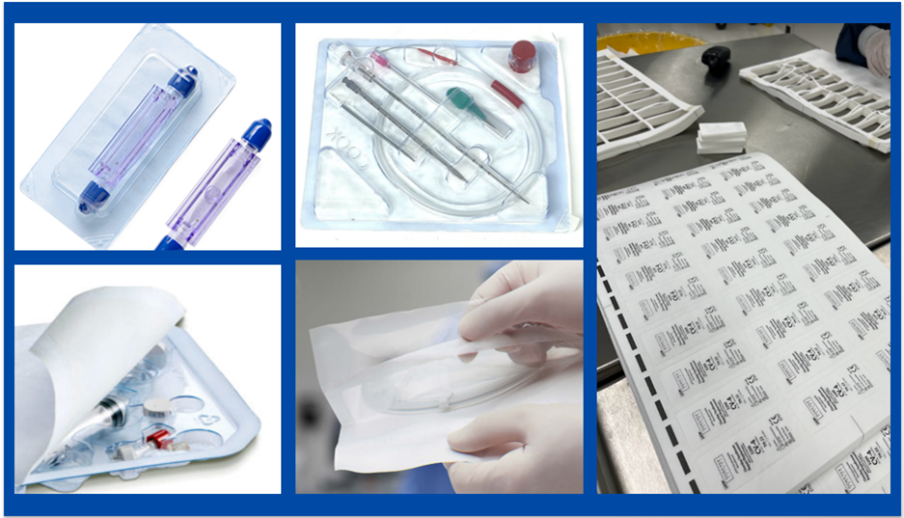
Working in the world of medical packaging, I knew we carried the responsibility of protecting medical devices and in turn the patients that need them. But that responsibility and understanding took on a whole new meaning for me with my daughter LillyAnn. My hope is by sharing her story with you, you remember that what you do is so much more than “just packaging” and that every decision you make has the potential of saving a patient and impacting a family.
The Day Everything Changed
Steve and I walked into our twenty-week ultrasound expecting an ordinary milestone; another chance to see the tiny girl we were already dreaming about. The ultrasound technician chatted easily while moving the wand across my stomach, pointing out tiny hands, long legs, and the gentle curve of a spine. Her voice faded mid-sentence, and I felt the shift immediately.
My background is in biology and biomedical engineering. I understand anatomy, and I understand what silence during an ultrasound often means. Her attention stayed fixed on one area. The heart. A quiet heaviness settled in my chest as I watched shadows flicker across the screen, trying to interpret shapes while my own heartbeat grew louder in my ears. Finally, she said gently, “I’m finished with the ultrasound. We’d like you to move to another room so the doctor can speak with you.” That was the moment I knew.
The Unknown
The doctor entered shortly after, wearing the careful optimism physicians learn to master. She explained that parts of the fetal anatomy, especially the heart, had been difficult to visualize and recommended evaluation with maternal fetal medicine specialists.
The fear truly began the moment we left the office. Like so many parents facing uncertainty, I did the worst possible thing. I researched. Within minutes, I was drowning in medical journals, parent forums, and heartbreaking stories. Infants undergoing multiple open-heart surgeries. The future I had imagined for our daughter began to fracture.
A Name for Our Fear
Weeks later, we walked into the maternal fetal medicine clinic carrying equal parts dread and hope. After some testing, our fear finally had a name: Tetralogy of Fallot. Tetralogy of Fallot is a rare congenital heart defect made up of four structural problems affecting how blood flows through the heart. Babies born with it can appear blue or gray because their blood carries less oxygen. During this visit, we learned that every child diagnosed with Tetralogy of Fallot would eventually need heart surgery and ultimately, lifelong cardiac care.
Hearing it was terrifying, and strangely … relieving. The unknown had become something tangible, something understood, and something treatable. Still, uncertainty lingered. Some babies require surgery immediately after birth. Others could wait months. We wouldn’t know our daughter’s path until she arrived. For me, from that moment forward, pregnancy changed. It became weekly monitoring, scan after scan, and a silent question at every appointment, is she okay today? Our delivery plans changed too, we were told delivery would need to happen at the University of Michigan, where specialists were prepared for babies like ours. Our lives slowly reorganized around a heart we hadn’t even held yet.
When Everything Changed Again
On November 10th, our daughter LillyAnn was born. As the medical team evaluated her, one encouraging update followed another. She was stronger than anyone had predicted, and for the first time in months, we allowed ourselves to exhale. Lilly wouldn’t need immediate surgery. Instead, doctors believed we could wait until she was bigger and stronger, improving her chances for a successful repair. Her surgery was scheduled for May.
For a while, it felt like we had been given the gift of time. But Tetralogy of Fallot comes with something called Tet spells, sudden episodes where oxygen saturation levels in the blood can drop rapidly and without warning. They’re something no one can truly prepare you for.
In February, we noticed something different. When Lilly cried, it wasn’t always her normal cry. These episodes were more intense, more alarming. Her body seemed to struggle, and the sound she made felt wrong in a way only parents can recognize. We started calling them “Lilly fits.” They happened a few times over the course of a week. Each time, our concern grew. Eventually, we called her doctor and explained what we were seeing. The response was “let’s definitely check it out”. At the appointment, they did a full evaluation. That’s when we learned the truth; Lilly wasn’t just having unusual crying episodes. She was having Tet spells.
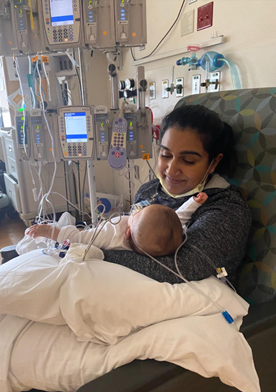
The doctor was honest with us. We might not have as much time as we thought before surgery. We were instructed to head straight to the University of Michigan Emergency Department. The cardiac team in Ann Arbor would be notified that we were on our way. When we arrived, Lilly had another “fit.” This time, the doctors saw it happen in real time. We were rushed to the back and monitors were placed quickly. Then we saw the number. Her oxygen saturation level was in the low 40% range, which to put that into perspective, any levels below 90% are considered clinically significant and potentially dangerous. In that moment, we understood we weren’t going to be going home anytime soon.
Lilly was admitted to the pediatric cardiac intensive care unit. Living in the hospital reshapes your definition of normal. A good feeding becomes a victory. Stable numbers feel like a celebration. Life shrinks to the size of a hospital room. That night the doctors met with us. After consulting with her surgeon, the decision was made that Lilly’s repair would happen the following morning.
The surgeon walked us carefully through every step of the procedure. As she described the patches and sutures that would mend Lilly’s heart, I thought about the long journey those tiny parts took to get to her—protected, sterile, and ready the exact second the surgeon reached for them. The surgeon’s confidence became something we held onto tightly. Handing Lilly over for anesthesia preparation felt impossibly unnatural.
Surgery was expected to last four hours. Then the first update arrived: the repairs were complete; she was off bypass and doing well. Hope entered cautiously. When the surgeon finally walked toward us, she smiled. Lilly had done beautifully. Her heart had been repaired; obstructive muscle removed, defects closed, blood flow restored.
Throughout recovery, once again Lilly proved stronger than we imagined and healing began to look wonderfully uneventful.
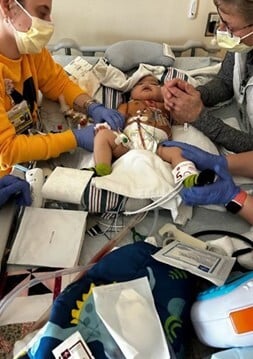
Going Home
After almost two weeks in the hospital, monitors were disconnected one by one and nurses said goodbye. Walking out of the hospital carrying Lilly felt surreal. As we stepped outside together, and one quiet truth settled in: our daughter’s story was only beginning.
This life event changed my understanding of my work forever. Medical packaging isn’t just packaging. It’s trust and reliability in the most critical moments. It’s the confidence we give doctors when seconds matter and lives are on the line. It’s the quiet assurance families never see—but depend on completely.
Somewhere, another parent is sitting in a waiting room, holding their breath while a surgeon works. They may never know our names. They may never see the pouch, tray, or seal that protected what saved their child. But what we do matters deeply.


