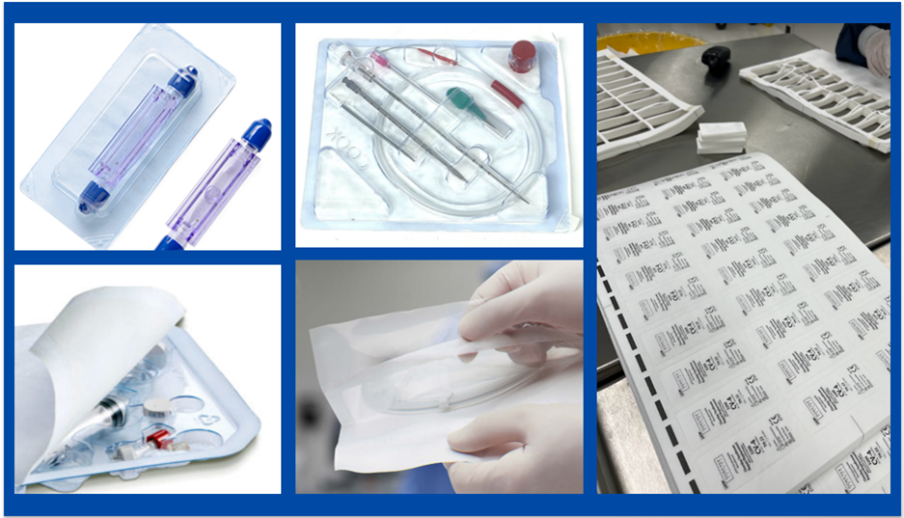
The Triple Packaging Principle: How Hospitals Safeguard Sterility While Advancing Sustainability
Sterile medical devices are essential for safe patient care. To ensure that these devices remain sterile from manufacturer to operating room, it requires a carefully controlled system of packaging, handling, transport, and storage. Once a device is delivered to the hospital they follow structured processes and use protective packaging to ensure device integrity and patient safety. In this article we will look at a typical device’s path in a Netherlands-based hospital from delivery to point-of-use and how hospitals in Europe are using their influence to help reduce packaging waste and support sustainability efforts.
The Triple Packaging Principle
Medical devices have three main packaging layers, all with their own purpose. This concept in sterile medical device logistics is the triple packaging principle, which includes:
- Transport packaging – protects products during shipping and logistics.
- Distribution packaging – used within the hospital for internal transport and storage.
- Sterile barrier system – the innermost layer that directly protects the sterile device.
Each level corresponds to different environmental requirements and contamination risks within the hospital workflow.
The Hospital Flow of Sterile Devices
When sterile medical devices arrive at a hospital, the process begins with a delivery check. Staff inspect transport packaging for damage, verify remaining shelf life, and confirm that all legally required information is present on the packaging layers. Products are scanned using barcodes that link to data systems, allowing hospitals to track devices in logistic systems and patient records.
After inspection, products are moved to stock storage, here they remain in their transport packaging. In storage areas, sterile and non-sterile goods may be kept in the same room but must be separated. Strict hygiene conditions apply; all packaging must be stored off the floor, away from outside walls, and in areas protected from pests.
Products typically remain in stock storage for 1-2 weeks, depending on the product type and hospital need. When needed, the devices will move to the central sterile storage department. Before entering here, the outer transport packaging (often cardboard or plastic) is removed in a designated area to prevent contamination of the sterile storage environment. This means the devices are stored in the central sterile storage area in their distribution packaging. Storage in this area is limited and therefore, products will remain here for only a few days prior to use.
Central sterile storage areas are highly controlled environments. Access is limited to authorized staff, and the rooms maintain positive air pressure with HEPA-filtered air to reduce contamination risks. Employees must follow strict clothing and hand-hygiene protocols.
From this central sterile storage point, devices are distributed to hospital departments using their distribution packaging and dedicated transport containers. Before use in the operating room, the distribution packaging is removed in a special preparation area, often within a laminar airflow zone. This controlled airflow minimizes the risk that airborne particles contaminate the sterile barrier system. Packaging materials such as wraps and plastics are usually separated for recycling in this room. The packaging of the sterile barrier system, the last layer of protection, is removed at point of use, in the operating room. Throughout the storage life of a device and before use, the packaging integrity and sterility expiration date are checked regularly.
Sustainability Challenges and Future Trends
When looking at the overall flow and use of packaging in a hospital system, it’s clear each layer serves a purpose in protecting patient safety. It’s also clear that while sterile packaging is necessary, it also generates large volumes of waste. While medical device and sterile packaging companies look at how they can reduce packaging waste before it enters the hospital, hospitals in the Netherlands and elsewhere are also exploring how they can contribute to being more environmentally responsible. Particularly when recycling medical packaging is not always straightforward.
Materials may contain multiple plastic types, and used packaging often contains large volumes of air, making transport inefficient. Therefore, hospitals are looking at how they can better recycle polypropylene packaging, and when appropriate, considering adopting in-house sterilization containers that would help to reduce disposable packaging. They’re also using their influence to push companies to consider more circular solutions such as reusable instruments, refurbishment of devices, and designing products with lower environmental impact.
Sustainability initiatives in Europe like national healthcare “green deals” and hospital green teams are helping to drive these changes. It’s no surprise to anyone that balancing sterility, patient safety, and environmental responsibility will remain a key challenge for healthcare systems in the coming years.