How One Patient’s Experience Became a Profession
It was 12 years ago this past summer, but I can remember it all like it was yesterday. I was getting headaches that were a stinging pain in the back of my head. They would come and go, and often with a quick movement the pain would change. I was also suffering from a stiff neck that I could crack repeatedly. Being only 13 years old, my symptoms were dismissed as growing pains by my pediatrician. We were told the odds of something actually being in my brain were less than 5%, so why do an MRI?
Fast forward a year, it’s spring break, my family is in Mexico. While I was painting a bowl, my mom noticed my hand had a severe tremor. It was concerning to her, so she called my doctor. At this point, his recommendation was that I go see a neurologist. The soonest we could get in was 12 weeks. Lucky for me, my mom was my best advocate and pushed until they could get me in within three weeks. For me, three weeks wasn’t soon enough. During those couple of weeks, I went from muscle spasms to staggering around when I walked to experiencing vision loss. Losing feeling in the left side of my tongue and feeling sick to my stomach were the final symptoms that made my mom take me to the emergency room before ever getting a chance to see a neurologist. I was immediately taken for a CT scan and MRI, where they found a tumor the size of an egg in my brain. I went from thinking I had growing pains to having a brain tumor in the span of 12 hours.
|
The white egg shape is my tumor, and the distinct white line behind it is where I was getting headaches from the constricted vein. |
I had emergency surgery the next morning to put in an external ventricle drain to help remove the cerebrospinal fluid from my brain. For the next six days, I had to remain completely level with the drain to ensure my brain remained at the correct pressure. At the time, the sophisticated way of ensuring this was using a small level taped to a yardstick. After six days, it was removed and the hole in my skull was sutured and superglued shut to prevent it from leaking.
Ten days after being admitted to the hospital they were able to do a biopsy on the tumor and I was officially diagnosed with brain cancer. After being diagnosed, I went through a port-a-cath placement, four rounds of chemotherapy, and 25 rounds of proton beam radiation.
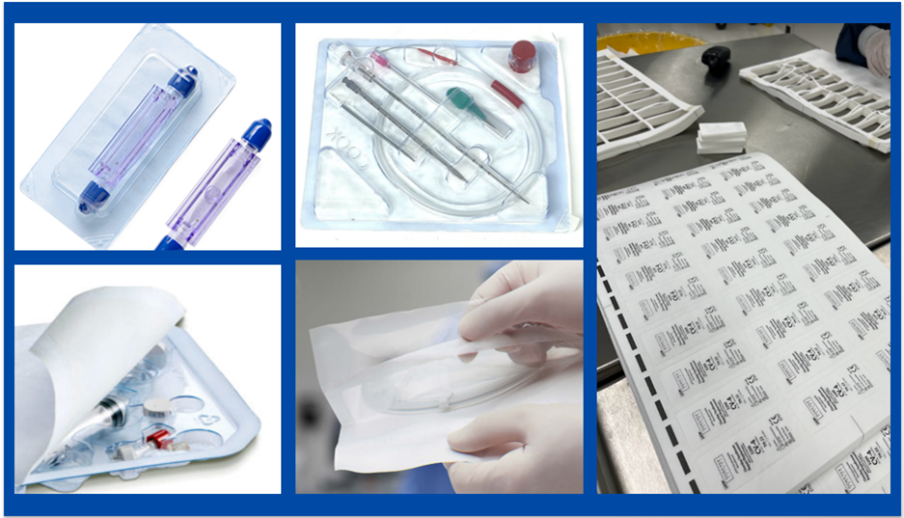
Hospitals are scary places, but even scarier as a kid. One thing I began to notice was how noisy the medical packaging was, especially when being peeled open. I eventually associated the sound of medical packaging being opened with pain. The crinkle of Tyvek and films caused my body to tense. By the end of my treatment, I was conditioned to think packaging crinkling equaled pain. It was this experience, and encouragement from my dad, that led me to majoring in packaging. I initially set out with the goal to completely change the materials medical packaging was made from. Now that I am in the industry, I know and understand that is not entirely possible, but I still believe a change needs to be made.
In hopes of finding a solution and creating a change in medical packaging, I’ve proposed a new charter as part of the aseptic presentation KiiP group. As part of this charter, I am recommending five phases: 1) receiving feedback from patients on medical packaging, 2) researching new improvements for packaging, 3) validating and verification, 4) submitting findings to FDA, and then 5) releasing our findings.
In the first phase of the project, our feedback will be specific to medical packaging that is used at a pediatric patient’s bedside. The decision to focus on pediatrics was simple for me—hospitals can be terrifying places for children, so any way that we can eliminate packaging from being an additional trigger is a win. My hope is that the data we can get from this research will allow packaging engineers to get more creative with their solutions and to customize the packaging for the patient. The wants and needs of a 10-year-old vs. a 60-year-old are significantly different. We design devices for specific demographics, so why not packaging?
Having been on both sides of the industry now, as a patient and a packaging engineer, I have advice for both sides. For someone going through a terrifying diagnosis like cancer, one thing that really helped me was positivity and the quote, “tough times never last, but tough people do”. I lived by this when I was first diagnosed and decided I was going to be one of those people that beat this. I also recommend finding someone or something that will make you smile or laugh. Laughter truly is the best medicine. To my fellow packaging engineers and medical device manufactures, please remember you aren’t just designing packaging and devices for the doctors and nurses of the world. Yes, they are your “end-user”, but so are the patients. Don’t forget to keep them in mind and to remember that the devices you design and manufacture are helping to improve or save lives!
On a personal note, I’m proud to share that I have since gotten over my association with pain and packaging. I am now a regular blood donor with the American Red Cross and have donated over 45 pints. I am even prouder to share that I have been cancer free for 12 years and can’t wait to be part of a team that makes lasting change to the development of medical packaging.