Why is the Sterile Field Important in the OR?
Regardless of whether you are new to the healthcare industry or an industry veteran, we’ve all heard about the “sterile field.” Thinking about the sterile field probably brings a few words to mind … operating room (OR), surgery, patient. Maybe you also think of blue gowns, gloves, and scrub caps. But what exactly is considered the sterile field, how is a sterile field created, and why is it important?
To understand the sterile field, one must first understand the aseptic technique. This technique was established in 1867 by a British surgeon, Joseph Lister (yes, Listerine is named after him). Doctor Lister was the first surgeon to perform a surgery using this aseptic technique. Since then, the technique has evolved. Today, there are several key components to the aseptic technique: barriers, patient equipment and preparation, environmental controls, and contact guidelines. Each of the four components mitigates risk of contamination in a specific aspect of the surgical preparation process. Strict and comprehensive application of aseptic technique in the surgical area and all it contains creates the sterile field.
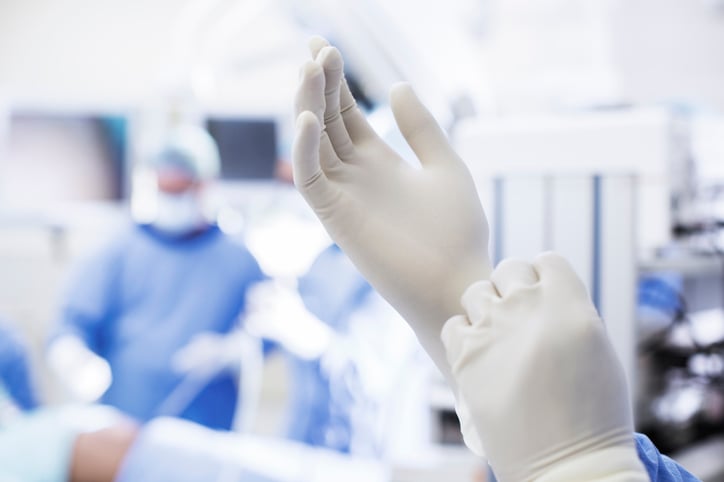
What is the sterile field?
The sterile field is a designated area in either the operating room (OR) or a clinical setting that has been prepared to be free of bacteria and particles (contaminants). Aseptic technique practices greatly reduce exposure to infectious microbial agents.
The sterile field includes trays, drapes, all supplies, as well as the patient, instruments and substances used to perform the procedure and all surfaces, such as operating table and trays. A surgeon or healthcare worker can only become part of the sterile field once they have “scrubbed in,” which means they have performed a surgical hand wash (more than just singing the alphabet) and have been properly gloved and gowned.
How is the sterile field created?
A sterile field is established with sterile surgical drapes (barriers) around a patient’s surgical site and on the table/tray that will hold the instruments and necessary surgical items. The most common practice is that anything below the patient’s drape is outside the sterile field. For a healthcare worker, they are considered sterile only from the armpit to the height of the sterile field’s surface and from 2 inches above the elbow to their wrist. Every human interaction with any of the surgical paraphernalia must follow precise techniques that direct how a package is opened, how the healthcare worker can safely hold or move the package, and how to maintain strict protocols on movement and actions within the sterile field from entry to completion. From air handling and circulation to washing methods, drape unfolding, getting into and out of PPE, and even limiting foot traffic, procedures are so precise, creating and maintaining the sterile field can seem as complex as the surgical procedure itself.
Why is the sterile field important?
The number one job of the sterile field is to protect the patient from a post-surgical infection. The Centers for Disease Control (CDC) estimates one in every 31 U.S. patients contracts a healthcare related infection. Data singling out statistics for surgical patient infections is not as readily available, due to variables in how data is collected. What is known, however, is that surgical site infections (SSIs) are the most common post-operative infection, affecting 1 in 24 surgical patients. Proper maintenance of the sterile field helps to minimize the number of surgical patients who will experience this statistic first-hand. In addition to protecting the patient, the sterile field protects healthcare workers from exposure to blood, body fluids, or other potentially infected material during the procedure.
Why should the packaging world understand the sterile field?
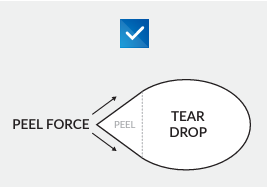
In sterile healthcare packaging, we design for aseptic transfer of the contents. It is a packaging engineer’s job to not only ensure the packaging delivers a device safely, but that it can also be transferred into the sterile field appropriately, without compromising the contents or the sterile field. Packaging factors that contribute to aseptic presentation begin with material selection. Other factors include the packaging system’s vulnerability to sterilization, strength limits to protect the device, microbial properties and even opening the package for use with fully aseptic transfer. Under the six degrees of separation theory, the packaging engineer is not that far from the patient receiving the contents of the packaging system they designed and validated. There are many reasons to pour precision and innovation into the work of every packaging system design. The chance to improve patient safety through completely aseptic presentation of the devices and tools we package is definitely a reason why all of us in the packaging world should understand the sterile field and how we impact it.
Sourceshttps://www.healthline.com/health/aseptic-technique#types
https://www.albertahealthservices.ca/assets/wf/eph/wf-eh-surgical-aseptic-technique-sterile-field.pdf
https://www.ncbi.nlm.nih.gov/books/NBK459175/
https://www.uptodate.com/contents/overview-of-control-measures-for-prevention-of-surgical-site-infection-in-adults
https://www.patientcarelink.org/improving-patient-care/healthcare-acquired-infections-hais/