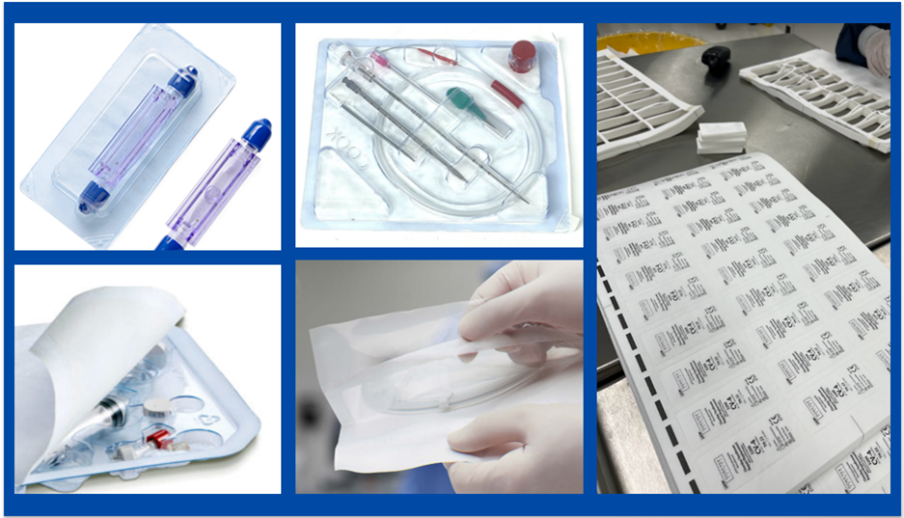
Can Packaging Postponement Find Its Way into the Medical Device Market?
As we all adjust to the "new normal" brought on by the COVID-19 pandemic, many medical device companies are doing the same. The downturn in elective medical and surgical procedures has upended our businesses. This begs several questions.
-
How can medical device companies adapt to this new normal?
-
What role can packaging play in this challenging transition?
-
What other trends are unfolding in the healthcare industry?
As many readers of this blog are aware, packaging is often perceived as an afterthought. Its importance and complexity can be underestimated. Regardless of perception, the reality is that the role, criticality, and ability to successfully deliver a sterile product remains at the forefront of product development.
Medical device manufacturers (MDMs) are putting increased resources and expertise into the development of device packaging. Market leaders now run product and packaging development in parallel. This parallel process often shortens the overall project timeline vs. waiting until the end to design packaging. Working in tandem can also lead to a more efficient packaging design that ensures adequate protection and sterility for the product inside.
Once a device is validated and released to the market, a standard production model of Manufacture, Package, Sterilize, and Distribute typically follows. While some unique distribution and configuration models may apply (i.e., consignment and procedure kits), most MDMs follow the standard model. Herein lies the potential: could challenging that traditional model create opportunities that help overcome market pressures? If so, benefits such as reducing costs, optimizing sterilization processes, and improving the sustainability of products may follow.
You might be thinking, "What is he talking about?" Or, "Changing the model? Way too hard and not worth it."
You're right about the difficulty; this is a complex undertaking. That said, the thought-provoking concept of "packaging postponement" is worth serious consideration based on the unique opportunities it may present.
Postponement is not a new idea, as explored in this 1997 Harvard Business Review article discussing Hewlett Packard's postponement operations model. While the alternative model hasn't taken hold in the medical device industry, its potential processes and benefits for sterile medical products bear further consideration.
A postponement model for MDMs could feature the steps of Manufacture, Package (primary/sterile barrier system only), Sterilize, Package (secondary/tertiary packaging), and Distribute. When compared to industry's traditional model, a postponement model would alter the flow by adding a second packaging step, which could present the following opportunities:
Optimization of Ethylene Oxide (EO) Sterilization Efficiencies
In many current EO sterilization processes, chambers are loaded with pallets stacked with tertiary packaging (often corrugated). The tertiary packaging contains secondary packaging (paperboard) that comprises the sterile barrier system and the device requiring sterilization. This standard process involves a high volume of packaging materials. Since both tertiary and secondary packaging materials are cellulose-based, they are likely to absorb some amount of sterilant. This, in turn, contributes to longer cycles and higher-than-necessary quantities of sterilant being used to achieve sterility. In addition, instituting a process that postpones secondary and tertiary packaging until after sterilization could help companies meet FDA sterile device packaging guidelines.
By postponing secondary and tertiary packaging operations, MDMs could load reusable totes that don't readily absorb sterilant. Moreover, pack-out optimization would allow more product units per load, deliver cost savings, and achieve responsible packaging consumption wins by eliminating tertiary packaging (which is often discarded upon receipt at the distribution center, anyway).
Furthermore, the postponement model could help companies optimize EO sterilization cycles and conquer other industry-wide challenges, as my colleague Dan Floyd highlighted in the August 12, 2020, posting.
Optimization of Sales Configurations
Another potential benefit of the postponement model focuses on improvements for medical device end-users. Packaging engineers often hear grievances from nurses and healthcare customers regarding the amount of packaging that accompanies devices. It is especially common to hear that the secondary package containing the sterile barrier packaging is often discarded upon arrival, so, " why bother sending it?"
While I recognize that protective secondary and tertiary packaging is needed to safely transport sterile products, delaying the addition of these packaging layers until after sterilization could allow for more customization and configurations based on that customer's needs.
For example, let's say a customer continuously orders 100 units per month of a particular product. This order requires distribution of 100 units in sterile packaging and individually packaged in 100 cartons. Alternatively, by applying a postponement model, the secondary packaging MDMs may be able to deliver that same product in a more efficient and optimized configuration that would work better for the customer. Improved packaging solutions could include cartons containing ten units (vs. one single unit) or, better yet, tertiary packaging robust enough to eliminate secondary packaging altogether (i.e., merely shipping the product in a corrugated box).
Sustainability
A third potential benefit of postponement is increased sustainability through more responsible consumption of packaging. Delaying secondary packaging achieves operational efficiencies in pack-out, while entirely removing secondary packaging leads to smaller unit sizes and more productive shipping configurations. These optimized processes may also increase sterilization throughput and positively impact the transportation cycle as well.
Furthermore, delaying secondary packaging operations may allow packaging systems to shed layers of protective packaging and product literature. Companies will be able to eliminate some secondary packaging materials as they optimize tertiary packaging and shipment configurations. Through these steps, both the medical device manufacturer and end-users may realize cost savings in recycling and landfill expense.
Regarding product literature, many companies are required to include instructions for use (IFUs) with each device. Depending on where that product is sold, the IFUs are likely translated into multiple languages, often creating a short novel to accompany each device. What if IFUs were added to each unit just before shipment, based on the destination? This would reduce material consumption through shorter, single-language instructions for another sustainability win.
Wrapping Up
Industry-wide adoption of postponement will by no means be an easy process to implement, nor will it work for every product or MDM. However, I challenge all of us in the medical device space to look at our product lifecycles and question our current models. As the healthcare industry works to adjust to the new normal while facing business disruptions, regulatory changes, and mounting environmental and sustainability pressures, packaging postponement practices could be a step toward creating and driving improvements and efficiencies in the healthcare space.